An old colleague of mine sent me her birth story recently. Here’s a midwife’s perspective on the birth of her beautiful baby girl.
I debated about whether to share this, but realised that sometimes it is cathartic to express yourself after going through a stressful time.
Basically, I started off with a VERY complicated pregnancy. I’m not going to go into details here, but it required hospitalisation and a lot of time off work until 20 weeks. Being a first time mum and a midwife, I found this time very hard mentally. I think many first time mums focus on the birth and concerns about that, but I was NEVER concerned about the birth. Being a Birthing Unit midwife means that I am well informed and would have been confident to make the best birthing decisions given whatever circumstances came my way! Ideally, I would have wanted a natural drug-free birth (while always being open to pain relief if I needed it), but my main concern would always have been the safety of my baby. From a midwife’s perspective of not always seeing happy stories, and a history of anxiety, I was burdened with worry from the beginning about getting through a pregnancy safely. 35 weeks + 5 days is a LONG time to be feeling constantly worried.
I had a few weeks where everything was going smoothly. I was having regular scans, and then at 29 weeks we found out that our baby had asymmetrical IUGR (intrauterine growth restriction). This means that the baby isn’t growing properly for gestation. I was at least thankful that it was the asymmetrical kind – if you have IUGR this is the one you want! It means that the placenta isn’t functioning optimally to provide nutrients, but the baby is preserving brain/head growth, resulting in other areas such as the abdominal circumference not growing well. The baby had dropped from having her abdomen growing at approx 40% to 3% in a matter of 3 weeks – so pretty drastic!
Being a full time midwife while having a complicated pregnancy is HARD. I know work is hard for anyone who is pregnant and working shift work or a physical job (or any job at all), but it is harder with complications! I was so thankful to have my manager and colleagues support me where possible. However, it is SO strange to be treating women who may have come in with a growth restricted baby and concerns about their baby’s movement. Obviously, I didn’t share my own story with them for professional reasons, but on some really busy shifts where I was on my feet all day, it was hard to deal with. I hadn’t even had the chance to know if my baby had even been moving normally on those days (which is really important in the context of IUGR).
Towards the end, the plan for my birth had been an induction at around 37 weeks. I was covered with steroids to improve baby’s lungs (thankfully – given she ended up being born early by caesarean section).
Steroids are given in 2 doses 24 hours apart. I had these on a Friday and Saturday as well as having CTG monitoring of her heart rate – both days this was absolutely textbook perfect. On the Sunday we sold our car and were meant to pick up our new one on Monday. We joked with the friend we sold it to on Sunday that we hoped we didn’t need it for anything on that one night. Well, it turns out we did. At about lunch time I realised that I hadn’t really been feeling the baby move much. I lay down and prodded and poked her myself and nothing was happening. I was thinking to myself “am I imagining things? / I don’t want to go in to hospital to be annoying,” but ended up deciding to have a large coffee. If her movement wasn’t normal in an hour, I would call my midwife to go and get checked. We ended up getting an uber into hospital sooner than an hour due to my gut instinct that something wasn’t right.
I knew as soon as I was put on the CTG that the baby’s heart rate was a lot different to the two previous days, and was abnormal. I got scanned by a doctor and she wasn’t moving on ultrasound either, despite being prodded quite vigorously. The labour ward was busy that evening and the doctors had to come in and out, but I knew what was going to happen when I was asked “when did you last eat?” by the doctor. My midwife confirmed that the doctors wanted to do a caesarean section, and asked if I was ok with that. My response was “I just want my baby out safely”. My poor husband was a bit shell shocked. I think that I subconsciously knew what the outcome would be going in that day if everything wasn’t ok, but he was completely surprised and had to very quickly wrap his head around the idea that our baby was coming!
I’m so grateful that I knew the doctors who saw me/performed my caesarean from working with them previously – it made that part a whole lot easier for me!
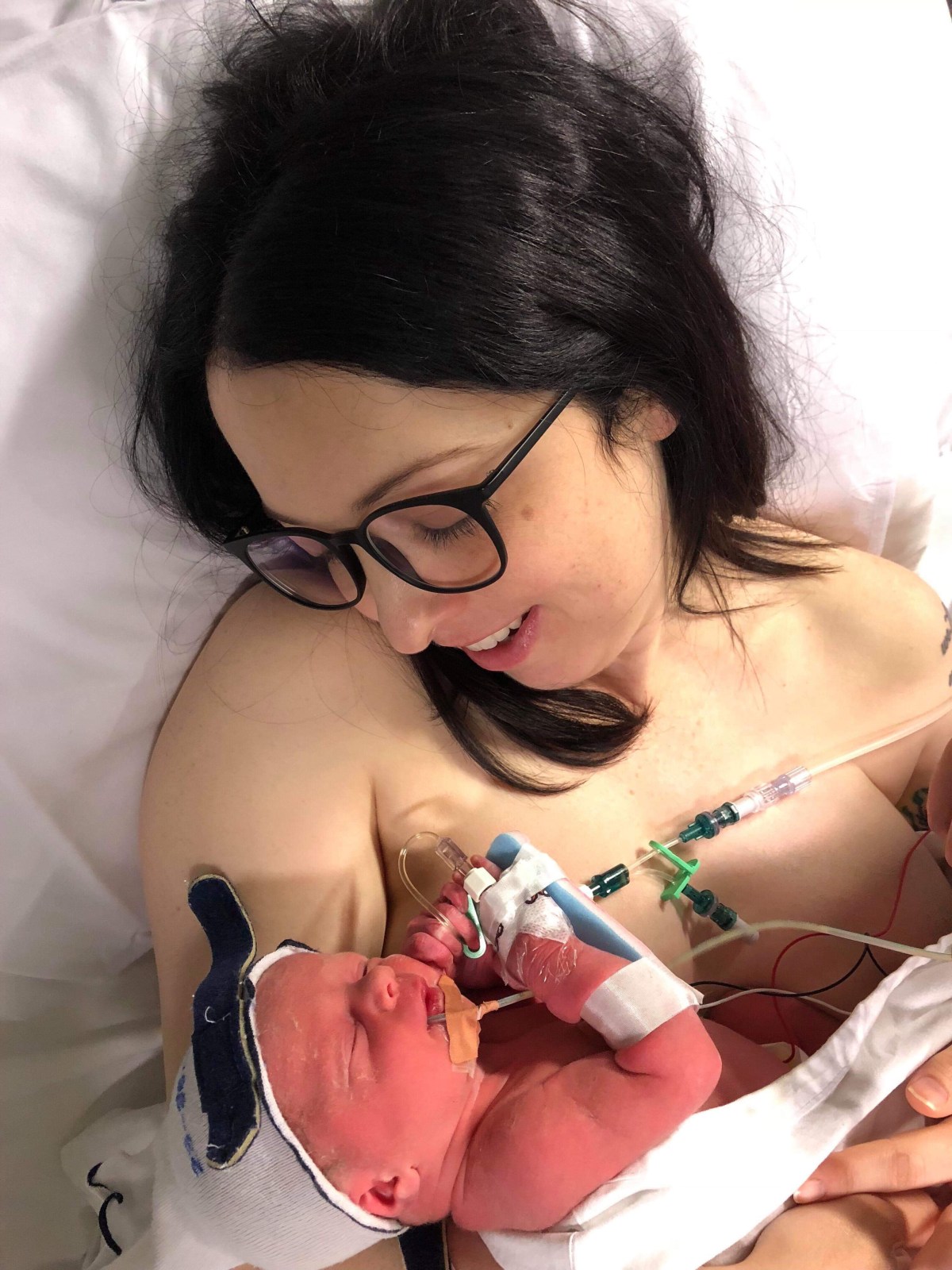
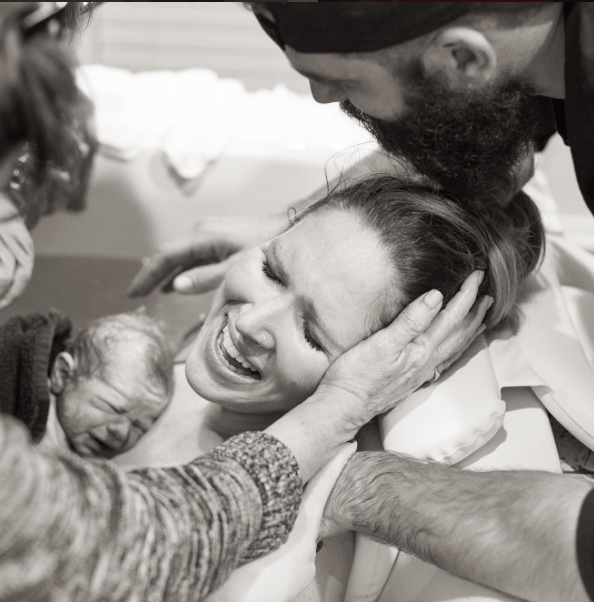
As soon as our baby was born it was like instant relief for me mentally – I hadn’t quite realised beforehand the extent that the pregnancy had affected me. Since her birth I’ve felt amazing. She did have to go to the nursery for 9 days because she was a tiny 2.166kg, and also needed help with her breathing for the first 4 hours. I wasn’t worried about this at all, because again from experience I knew she would be absolutely fine, and my husband got to go with her to the nursery.
I was so grateful for the amazing support I got in hospital. I was expecting to not see her until the next morning when the anaesthetic had worn off and I could walk. However, the midwife looking after me arranged for me to get taken down in my bed at about 3am when she was off the breathing support, and we got to have our first cuddle. There is truly nothing better than the first cuddle with your baby!
Take home messages:
Maternal instinct is so important! I’m even more aware of how important fetal movements are after this experience. I went in 3 times in the pregnancy with movement concerns (while being a typical midwife and second guessing myself for fear of being annoying/creating a workload). I went in first at 26 weeks, and it was at the next scan that she was found to be IUGR. The second time was at 32 weeks after I’d had a lot of vomiting. I knew the reduced movements were dehydration related, but I still needed to get checked out. The third time was when she needed to be born!
I think more can be done to support the mental health of women with early pregnancy complications. It is a really lonely and scary time being in limbo.
I think there should be a discussion about leave entitlements for working women with pregnancy complications. I have always been vocal about maternity leave rights for women before I was even pregnant. We have created a capitalist society that requires 2 incomes to service a household, and for women to also support the economy. Women don’t choose complicated pregnancies. If women do have complications, I think there should be leave entitlements that don’t require them to use annual leave or leave without pay. I don’t buy into opinions of “it’s your choice to have a baby – deal with it”. As I’ve said before, there would be riots if women went on strike and stopped having babies.
Was my birth experience positive given the circumstances? YES! I feel like I recovered really well from the caesarean. The only thing I didn’t like was the spinal anaesthetic. The actual procedure was completely fine, but it is the weirdest feeling when you go completely numb from the waist down.
Would I do it all again for our daughter? YES!!!