I stumbled across a statistic from SANDS, the Australian miscarriage, stillborn and newborn death support program a while ago. It stated that ‘Australian women are more likely to experience a miscarriage than to experience breast cancer’. Breast cancer awareness and information is everywhere and I know I’ve spoken with family and friends more about breast cancer than miscarriage. So as women, by not talking about pregnancy loss, are we making, what is statistically a horrible yet common occurrance harder?
In the past few years, I have spoken to women and been with women that have lost babies; early and late in pregnancy, but what I have found is women explain; the lead up to it happening, why it happened, how it happened, the procedure that was involved afterwards, but many do not discuss the emotional impact that it had on them and their partner. So today we’re talking about the unimaginable, yet more common that you think; grief and loss of a baby.
Finding out your pregnant is a life moment, that for many families will evoke happiness and excitement. For 1 in 4 women* in Australia, these women and their partners experience the loss of their baby early in the pregnancy. The first 12 weeks of pregnancy is when some families decide to stay tight-lipped about their newly growing addition (this being the time in pregnancy with the highest chance of miscarriage). So because the pregnancy hasn’t been announced, many couples grieve together in silence.
A less concealed grief for mothers and fathers is that of a stillbirth. 6 babies are born stillborn everyday in Australia, a statistic 10 times higher than SIDs related deaths.
Working within a maternity unit I’ve been exposed to some very sad situations, that you wouldn’t wish on anyone. My family and friends also, have not been immune to such loss.
I think many of us shy away from talking about topics like miscarriage, as well as telling people about being pregnant (within the first 12 weeks), because of how it then positions us for vulnerability. Vulnerability is an emotion that makes us human and has the ability to foster connectedness. We, as women, need to speak about the hard stuff surrounding pregnancy and not see loss as personal failure. At the end of the day, good friends only want the best for you and would move mountains to help you through the tough times.
Someone dear to me, whom will remain anonymous, has kindly written her story and the ways in which multiple miscarriages affected her, her relationship and her journey to two miracle babies.

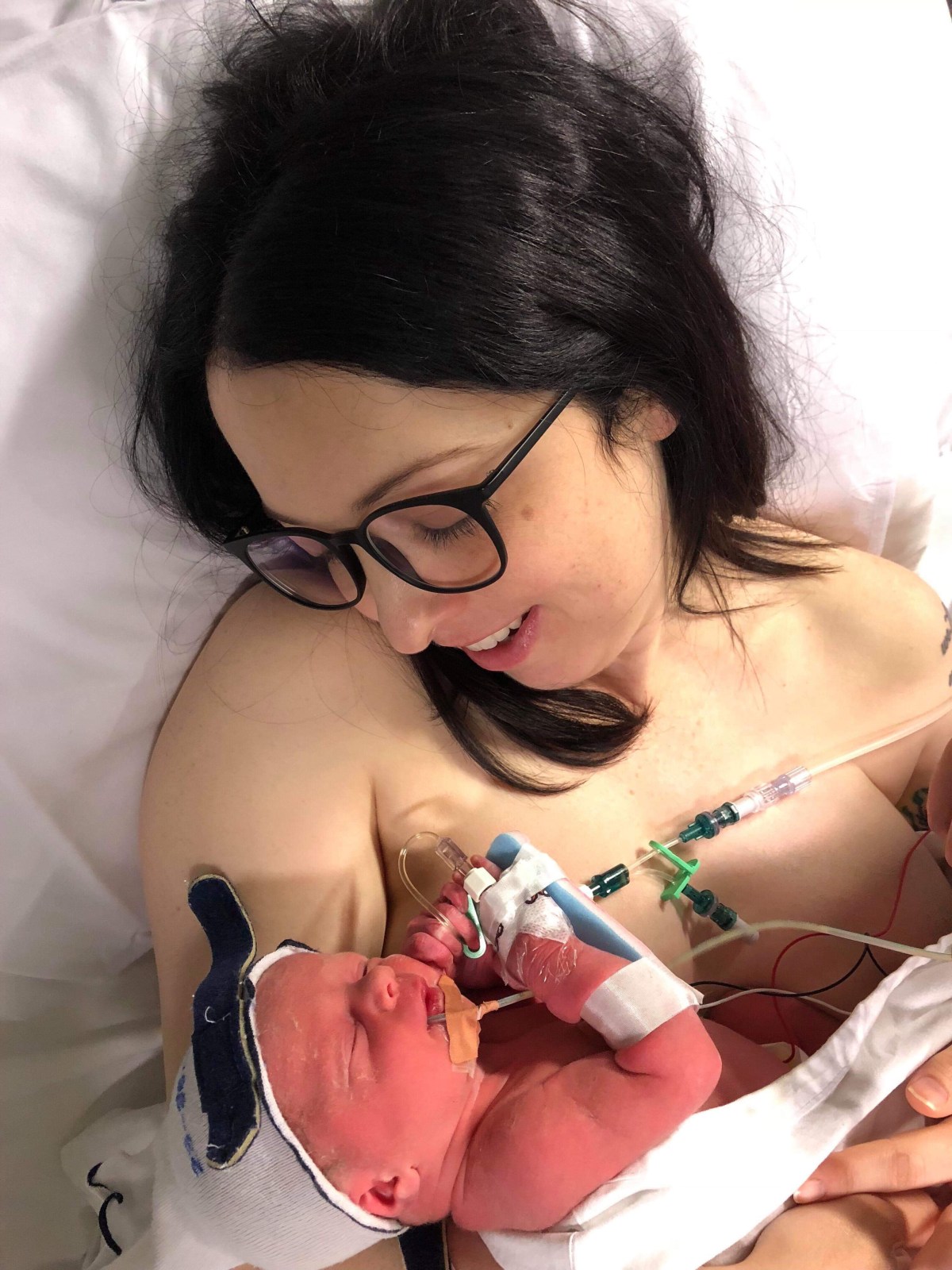
This is her story, “Little Miracles”:
To those who are going through or have been through a miscarriage, my heart goes out to you. I hope my story can give you hope and somehow help you heal.
To the partners who are trying to support their wives or girlfriends through pregnancy complications: know that you are doing a good job, and that the most important place you can be through all of this is with your partner, together. You are part of the equation and the difficulties of miscarriage or loss will affect you too. Make time for appointments, talk about how you are feeling, and when you can’t talk, sit in silence, and have your shoulder ready for the tears that will come.
To those who have a friend or family member experiencing pregnancy difficulties related to conceiving, miscarriage, or traumatic birth experiences: your support may go unrecognised at the time, but it is not unwelcome, and it will be appreciated.
Pregnancy. You think it’s going to be easy, but sometimes life can throw you a curve ball when you least expect it. When I was a child, I imagined my future as an adult with a good job, a nice house, a loving partner, and with children. Never did I consider how differently things could turn out, but as I learned, it’s important to expect the unexpected. I have two children, but I was pregnant eight times. We lost eight babies, as I was twice pregnant with twins. This is the story of my long journey towards motherhood and parenthood.
At the beginning of 2004, at the age of 23, my partner and I got engaged, and we decided to try to fall pregnant right away. With so much to do in preparation for the wedding, it was not until after five months of trying that I began to worry something was not quite right. I had stopped taking the pill months earlier, but I still had not had a period. My cousins had experienced problems having a baby, so I began to worry that I might find myself in a similar situation. I discussed this with my mother, who told me not to worry. She hadn’t had any problems, so why would I? I’ve always looked up to my mother and listened to her advice. I wanted to believe everything would be ok.
After another four months, when the situation had not changed, I decided to go to see the doctor. I was surprised, but relieved, to hear that it was quite normal for your periods to be irregular after coming off the pill and so, trusting the doctor, I decided to wait a while longer before becoming too alarmed. When a year passed, we decided it was time to start investigating things further. I am not sure if it was my age or my inexperience, but at that stage, the words “gynaecologist” and “obstetrician” meant absolutely nothing to me. I was referred to a gynaecologist/obstetrician, who was chosen by my local GP. I didn’t know it at the time, but this was the person who would become an integral part of my journey and who would eventually help save my life.
I was not exactly sure what to expect on that February morning in 2006 when we went to the appointment to discuss our infertility. Imagine our disbelief when a routine ultrasound revealed we were around seven weeks pregnant. I don’t know who was more surprised – us, or the doctor who had never seen us before. The rest of the consultation was a blur. I was so excited, I just wanted to get out of there so that we could ring everyone we knew to tell them the good news. After all, why wait? I was pregnant, and in my mind, fertility issues were about being able to fall pregnant. I wanted to tell the world!
Family and friends responded with joy and enthusiasm to the news that I was pregnant. No one was happier than my mother-in-law, who was expecting her first grandchild, and my parents, who were beginning to secretly worry that infertility might be an issue.
From the moment we knew we were pregnant, we began to plan for life with a baby. The list of discussion topics were endless, and an onlooker would have believed we were trying to make every decision about the baby’s life in the first few weeks of the pregnancy. We were so excited, why would we worry? I was a school teacher and I even told my class. It was a Friday afternoon and I was teaching when I felt that something was not quite right. I had to go to the toilet, but there were only 20 minutes left of the school day, and I had planned to go home straight after school, so I decided to wait.
By the time I got home, I was busting and raced for the toilet. To my horror, I saw it was filled with blood. If you have ever been in that situation, you will know the feeling. It is like the world has completely stopped. You don’t want to believe what you are seeing and for a moment, you panic.
We raced to the doctor’s surgery first anyway, only to then be sent to the emergency department. It’s funny how each miscarriage brought with it the same protective maternal response: if I get to the hospital straight away, everything will be ok, the baby will be ok. I was in quite a lot of pain by then, but had visions as we were driving of the doctor telling us everything would be ok. I wish I had been right. We were left in the hospital waiting room for what felt like an eternity. People came and went and I was still waiting, bleeding quite heavily. Looking back, it is quite disgraceful that you can be made to just sit in a hospital waiting room while you are losing a life inside you.
Finally, I was taken in to see a doctor, who told us the worst. A scan revealed the baby had passed away. I was 11 weeks pregnant. There are simply no words to describe the lonely moments soon after you realise you have miscarried a baby. You wonder what you did wrong and start to think to yourself, “If only I had or hadn’t…” about all the situations where you didn’t completely follow the rule book.
The only people in the world I wanted, besides my husband, were my parents, who were away and out of phone reception. I wanted to curl up in a ball and never come out. All our planning came crashing down around us. All the excitement of holding our first born in our arms was ripped out from under us. Surgery was planned for later that evening, and when 8:00pm came, my husband was asked to leave. “Visiting hours are over and tell your wife she can’t use her phone,” the nasty nurse barked as she went on with her shift. I found it ridiculous that my husband was being sent home. We were both grieving. We had lost a child. I was completely empty. Surgery came and went, and when I slept that night, it was as if I was still pregnant and the frightening ordeal was behind me.
Despite the number of miscarriages I had after that, I still believe the first was the hardest. While each additional loss brought with it the same grief and distress, the naivety from my first miscarriage had been stripped away. That first devastating loss was a wake-up call that complacency was not an option when it came to pregnancy. It was becoming more and more apparent that a magical combination, and a lot of luck, would be needed in order to conceive once again. Within a matter of months, and after taking medication for polycystic ovarian syndrome, I found out I was pregnant again.
The end of that year brought with it a lot of excitement as we neared the 12-week mark. Things were going very well and I attributed this not only to being more relaxed at the year’s end, but also to the fact that I followed every rule in the book when it came to what to eat and how to care for myself.
Nearing the end of the first trimester, I had a feeling something was not right. As soon as I went to the toilet, I knew we were losing our second baby. Quickly, we got into the car and were on our way to the hospital again. I was in a lot of pain, and while I wasn’t left to wait in the emergency waiting room this time, I was given a bed in a corridor, where I was left to wait for hours.
Finally, a midwife came and confirmed our worst fears. We would need a second dilation and curettage, known as a D&C, to “scrape the baby out”. I don’t know what was worse, knowing that I had lost another baby or hearing that my baby, who we had dreamed of and looked forward to meeting, would be “scraped out”.
The moment of going into theatre was one of sheer panic. Overwhelmed with sadness and unable to speak, I would simply nod and shake my head as the nurses, doctors and specialists would come to talk to me. Once the operation was over, we drove home with barely a word. Nothing either of us could say would bring back our baby.
While the first miscarriage was the hardest, the second brought with it a feeling of guilt and blame. As I was trying to process why this continued to happen to me, the guilt my husband and I felt began to cast a dark shadow over our marriage. We found ourselves unable to pick ourselves up out of the depression that the loss of two children had caused, and our inability to talk about how the miscarriages were affecting us individually and as a couple was having a devastating effect on our relationship. The problem was so great that talk of divorce even reared its ugly head.
In March 2007, I decided that I would give it one more month. Barely a week later, I found out I was pregnant again. I didn’t know how to tell my husband, but I came across a little shirt with a giraffe on it that read “I’ll be this big one day”. I wrapped up the shirt and took it out one night at dinner. We hoped and prayed for nothing more than the birth of a healthy little baby at Christmas. As quickly as I had decided that divorce might be the only option, our focus once again became the baby. Planning consumed us. If only life was as simple as wishing, hoping and praying in order to achieve your dreams. I read all the books and ate everything right. We were determined nothing would go wrong.
In late April I began to bleed again. I knew that three miscarriages was concerning; I wanted to know why this was happening to me – there had to be a medical reason. My theory was that I was miscarrying boys. I am not sure why I believed this, but probably in my frenzy of googling each time I fell pregnant, I’d somewhere read that your body can miscarry one sex. It was many years later that I learned that I had by then miscarried two girls, while the third was not tested. The late night scan revealed our worst fears. Our baby had passed away. Another devastating miscarriage. Another heartbreaking D&C.
A serious change was needed. One month is the time it took for us to find a block of land and a house to build on it. One week is the time I spent feeling sick before I decided to see a doctor. One minute is the time it took for the doctor to convince me to take a pregnancy test, while I told her, “I think I would know if I were pregnant, I have had three miscarriages”. One second is the time is took for the positive line to show up on the pregnancy test. I broke down. I didn’t want to be pregnant ever again – I couldn’t face another miscarriage. We didn’t know it at that time, but that cold day at the end of July was the beginning of what would become our official entry into parenthood, confirming my pregnancy with the little girl who would become known as T.
We were thrilled to learn at our 18-week scan that out baby, was growing well, was a little girl. At this time, I found out I had placenta prevue, a low-lying placenta blocking the baby’s exit, which meant that T had to be born by caesarean. I was booked in to have her at 37 weeks, on March 10, 2008.
“She is tiny,” I said to the doctors as I looked at the beautiful, perfect bundle in their hands. Weighing in at 2.4kg, T certainly was very small. I was able to hold her briefly before the paediatrician took her. The obstetrician focused his attention on the placenta. After quite a bit of prodding and poking, I could tell something was wrong.
“What’s the matter?” I asked as he spoke quietly with the midwives. “N, don’t panic, but the placenta is not coming out quite as easily as it should”, he replied. “It has left a relatively small hole in your uterus, which could cause future miscarriages”. I was too happy to care. The problems this hole could cause was not in my foreseeable future. My daughter was finally with us.
We certainly were not expecting to fall pregnant quickly, but less that five months after T’s birth, we found out we were pregnant again. Our excitement was short-lived, and later that year, we again lost the baby we had hoped to welcome. After that miscarriage, we decided that we would have a plan for more children, but if it never happened, we would enjoy our life spoiling T and that would be enough.
Our loss after T’s arrival was easier to deal with than the previous had been, but the miscarriages that followed were extremely traumatic and ultimately cost us our marriage.
In December 2008, I was pregnant again, and things were going smoothly. Then, without warning, another miscarriage came on. I knew that I needed to get to hospital and I called my husband, but having been through the drill so many times before, he simply said, “I’ll come after I finish work.” It was as if he didn’t realise I needed him. I felt so scared, sad and aIone, and if it hadn’t been for my brother-in-law, who raced from work to come and meet me, I wouldn’t have been strong enough to face another daunting surgery.
The effect each heartbreaking miscarriage was having on my body, our relationship and our ability to communicate with each other, was getting worse. I fell pregnant again a little over a month after the fifth miscarriage, and by this time we both felt completely drained. Then on a trip interstate, I began to feel unwell. I was sure we had miscarried. To our surprise, we saw that I was pregnant with twins, and that there was still one heartbeat. I didn’t even know I had been carrying twins, and it was bittersweet to realise that one baby had passed away while the other little fighter still had a good chance.
“You have a very good chance of carrying this baby to term, N,” the doctor said. “To give it the best chance of survival, you should take these progesterone pessaries. I will send you a script straight away. I suggest you arrange to get them immediately.”
I took some time off work to rest, and took the progesterone religiously, but just a month later, in April 2009, I felt that all too familiar feeling. When our worst fears were confirmed, it was decided that I would have a D&C two days later.
In the weeks that followed, I was completely and utterly grief-stricken. My husband buried himself in work and in the television; I had no concentration span and my thoughts were constantly drawn back to our lost babies. I hit rock bottom and was so distraught that on many a night, I would lie in bed sobbing to the point of hyperventilation. I felt sad, guilty and useless for not being able to protect our innocent children. It felt like no one could understand my pain, and though a handful of people asked how I was going and encouraged me to talk about my feelings, I had no strength, no motivation and no urge to tell them how I really felt. I had many friends, but I felt like I didn’t have anyone to talk to who would really, truly listen or take the time to understand. The one thing that made me feel safe and loved was when someone would take me in an embrace and just hold me, letting me cry if I needed to.
T was a blessing, arriving after three miscarriages and just as we began to believe we might never have children. But it is S, my youngest daughter, who was a real miracle. Neither she nor I would be here without the help of expert medical care, and a lot of love and hope.
After seven pregnancies and one beautiful daughter, it became clear that a break was needed. We fell pregnant in early 2010. I knew I was pregnant instantly. It’s strange, but having been pregnant so often before, I had a feeling from very early on that I must have been pregnant, even though for weeks the tests returned negative results.
After seven hours of driving on our way to go camping, I asked my husband to stop on the side of the road. I had packed a pregnancy test and was determined to do it then and there. We were on a dirt track and it was dark, so my husband’s job was to hold his phone as a light, while mine was to ensure I didn’t miss the stick – after all, I only had one test. Sure enough, it came up straight away: two clear blue lines. I was pregnant. We got back into the car without saying a word and continued to drive. There was none of the excitement you would expect with parents so desperately wanting another child. We sat in silence, knowing we would be facing yet another uncertain time. I turned to him and said, “This time, I need you in the hospital by my side if we miscarry. I cannot do it again. I cannot take another miscarriage, so this will be the last time I will be pregnant.” Silently, he nodded.
A few weeks later, I felt that all-too familiar gush. My heart sank. The emergency department was a blur. We knew the night would be long and that yet another D&C was on the cards. Luckily though, we went for a last-minute scan. As we sat in silence, the ultrasound technician carefully examined my uterus. She could see that we had lost a baby from the bleeding and that there was no heartbeat. She was friendly enough and was sympathetic as she gave us the news. She continued to scan me as part of the routine, when all of a sudden, there was a tiny glimmer of hope. A very dull flicker on the screen, almost impossible for the naked eye to see, signalled that perhaps a baby had made it and was still alive. Sure enough, the ultrasound technician measured the heart rate: 82 beats per minute. She confirmed that I had again been pregnant with twins and that one of the babies still had a chance. Anything under 80 beats per minute would almost certainly have meant miscarriage of the second twin too, so there was no point getting our hopes up yet. Losing twins just weeks apart the year before had taught us that there was no certainty. There was nothing to do but wait.
We were referred on to the hospital’s early pregnancy unit, a section dedicated to women in the same position as me, where I went for another scan a week later. There was a dedicated nurse, sonographer and doctor, and it was the first time someone actually took the time to listen to the story of my pregnancy difficulties and acknowledged the road I had come down. It was the first time someone had stopped, looked at me and said, “Can I give you a hug? What you have been through is simply tragic,” and I knew then that I was in good hands. After telling the nurse about my history, it was time for my scan, and there was still a heartbeat, now even stronger than the previous week, at 110 beats per minute. We were still not out of the woods, but we were making progress. Two older male doctors who were in the scanning room excitedly told me that they had found a good heartbeat, and to their surprise, I burst into tears, not daring to say anything.
Determined to help and give me hope, the excited and optimistic nurse explained about a controversial treatment in Queensland, Australia, that I would be a candidate for. Although it would require injections twice a week of the hormones HCG and progesterone, in addition to fortnightly blood tests, the treatment had been proven to work quite well in the USA could potentially help me keep the baby safe. He was always busy, but the nurse seemed confident she could get me an appointment via another unit at the hospital.
Within an hour, I had dropped my friend home, picked up my husband and was driving to meet the man I now call “the baby doctor”. I attribute the successful continuation of this pregnancy to the early pregnancy unit, the second unit at the hospital that helped get me the appointment, and to this doctor, whose decision to give me an emergency appointment for the same afternoon was, I believe, the turning point in the pregnancy.
Fortunately, this doctor was the answer for us. In just one day at the early pregnancy unit with him, I learned more about pregnancies and miscarriages than I had in the previous six years of problems. Understanding more about progesterone’s ability to prepare the body for pregnancy and the supporting role of HCG gave us the confidence to continue, and continue we did, as a scan seven days later revealed the baby was growing and had a heart rate of 182 beats per minute.
Everything was going smoothly with the pregnancy until 2:00am on Thursday 30 September, at 30 weeks and two days, when I got sharp pains in my abdomen and through my cervix. The pains in my abdomen were quite similar to those I’d had when I was miscarrying, but the pains in my cervix were completely new. Within an hour and a half, we were at the hospital in the labour and delivery ward. The midwife and doctor decided that I was not contracting and that the baby seemed happy. I was told it was quite normal to feel the pains I described, and that it was just my ligaments stretching.
No ultrasound was performed and I was so confident the doctor was right that I accepted this explanation and went home. I was warned that if I began to bleed or to feel contractions, which I had never felt before as T had been born caesarean, I would need to go back to the hospital.
My instincts started telling me something was still not right, and two nights later, I began to bleed quite heavily. It was 1:00am and once again, my toddler and husband were fast asleep. A good friend who lived nearby was still awake and was able to come to hospital with me. Not wanting to risk driving 80km, I decided to go to a closer hospital this time, and upon arrival, I was taken immediately to the labour and delivery unit. The obstetrician on duty insisted on doing an internal examination while we waited for the sonographer on duty to come to do a scan. With clenched fists, gritted teeth and tears pouring down my face, I let them perform the examination. Internals for me represented one thing – miscarriages. Needles I did not mind, operations I could handle, but those silver shiny “salad tossers” were a completely different story – they represented the babies that I had never met. The internal revealed that my cervix was closed and the scan revealed that I had grade four placenta praevia, a condition where the placenta is low-lying and covering the cervix, preventing the baby from exiting the birth canal. From what I could find out on the Internet, this condition was highly problematic, and bleeding could signal a rupture that could very quickly prevent oxygen getting to the baby.
Bed rest in hospital is something you read about in pregnancy magazines. You wonder what it must be like to sit around in bed in your pyjamas all day long, trying to keep your baby safe. The days blended into one another and the nights became a blur. I was the only antenatal patient on bed rest over the three weeks I ended up spending there. Although I could hear cries, I rarely saw any babies or had the opportunity to speak to the new mothers who were in the rooms surrounding me.
During my time there, I quickly learned who my really close friends were. Despite their own busy lives, there were a number of people who supported me and came to keep me company. Being in hospital was also a hard time for my husband and daughter. We lived a long way away, and my husband started work at 6:30am and finished around 4:30pm. There was a fine balance that we wanted to maintain between him visiting me and caring for T.
There was a mothers group within the unit. I was encouraged to attend by the midwife and couldn’t help but accept her invitation and nervously made my way to the common room, where I was surprised to see a bunch of other pregnant women all bustling in the room, some talking, others who were new like me, shyly waiting to see what would happen next. As we sat there, I looked around, trying to guess how far along everyone was and wondering why they were stuck in the ward on bed rest. These strangers, who I might not have met or befriended at any other time in my life, would become some of my closest, most trusted friends within a matter of weeks. Little did I know that they and a handful of other people I met at subsequent meetings, would become the people who would help my post-operative journey towards recovery, both physically and emotionally. To this day, I still keep in contact with these women, some of whom had twins, others who had babies at 26 and 29 weeks.
My doctor monitored my daily, sometimes twice daily if he happened to be on the ward. Placenta praevia continued to show up on the scans, but I think it was the pelvic pains that most concerned him. I was send for an MRI. It was the 5th of November, when I received a call from him.
He told me that the scans showed placenta percreta and this was the worst form of placenta accreta, where the placenta invades the uterine wall and can attach to other organs. I had been told in the past that a caesarean hysterectomy might have been on the cards, but I was not ready for the news that this was now not simply a possibility, but a necessity, in order to save my life, due to the risk of haemorrhaging. A team of medical experts had been called in to ensure the safe delivery of S a week earlier than planned, on Tuesday 9 November, at 36 weeks. Words like “coma”, “cell saver”, “general anaesthetic” and “intensive care unit” came up again and again. S and I would each face our own set of challenges at her birth, with her prematurity and my chance of blood loss, but there was no changing the situation and no escaping it either. The nightmare possibility of a massive bleed which could lead to death or an extended period in intensive care haunted me. I sent messages to my close family and friends and let them know the exciting news that S’s birthday would be a few days later.
I don’t remember much about the surgery itself. I have flashbacks of the buzz around the room as I was being prepared, and of a midwife wiping anxious tears from her face. But everything was okay. S and I were alive and well.
Pregnancy for me represents so many things. It represents family, new life, treasured friendships, hope, pain and grief. It is a mixture of many emotions that have significantly shaped who I am today. Had I not encountered the experiences of those six years, I doubt I would be the same person I am now. It’s hard to talk to friends and family about the pregnancies and the difficulties, unless they are experiencing or have experienced similar grief, but I feel so blessed to have come out of the experience on the other side.
While the pain of the miscarriages will never be completely gone, my excitement and love for my two beautiful girls makes up for it. I am wiser for the experience – and while I wouldn’t have thought it at the time, I recognise it now – a better mother.
*Calculating the rate of miscarriage is extremely difficult, due to the fact that many miscarriages happen even before the woman knows she is pregnant. Estimates miscarriage rate according to SANDs (miscarriage, stillborn and neonatal death support) of all ‘diagnosed’ pregnancies: 25% (or roughly 1 in 4)
At different stages of the pregnancy, the loss of a baby is classified differently.
-miscarriage – first 19 weeks or <400g
-still born – after 20 weeks or >400g
-neonatal death – first 28 days of life
Resources:
SANDS
Stillbirth Foundation Australia