So many of you have shared your birth stories with me, and I’ve been blessed and honoured to have witnessed many strong women and their families become mamas and parents – so it seemed like a no brainer that I would one day share my journey in becoming a mama with you guys, and what a journey it was!
When thinking back chronologically on the two day saga I couldn’t have imagined the rollercoaster of twists and turns that were ahead for me. I did know this was a possibility heading in, which definitely made it easier mentally, but boy was it looooong. And yet, looking back, I’d say I have an amazingly positive birth story, and loved the wild ride it took to meet Syd.
TUESDAY FEBRUARY 20, 2018
40 weeks and 5 days in the throws of a February heatwave, a woman can only handle so much thigh chafe before shit starts getting real (TMI?). I’d had a couple of stretch and sweeps, was 3cm dilated and over it! I booked in for some labour inducing acupuncture with a fabulous woman in Brisbane (if you want her details, DM me on Insty), and a few hours later started feeling niggles.

That afternoon I started having regular, but not strong, tightenings lasting 50 seconds straight off the bat. I could talk, walk and smile through them so I did my best to ignore them and we went for our regular 9pm walk (to beat the heat!).

When I got home they ramped up. The were 3 minutely, lasting 50 seconds and I had lots of back ache (munchkin was direct OP, meaning his spine was on my spine, not ideal). My midwife was kept in the loop and the plan was to call when I was ready to come in to be reassessed etc…..
WEDNESDAY 21st FEBRUARY, 2018

4am rolled around, I hadn’t slept and I was ready for either some pain relief, a good ol’ bath, or something! I was assessed at 6am in the Birth Centre at RBWH and was STILL 3cm and effaced (kill me), his head was very low (good!). My contractions had not increased in strength but were lasting a good length and still 2-3 minutely, so we decided to break my waters and get this show on the road.
It worked a treat – contractions stayed consistent in timing and length, and improved in strength.
I laboured in the shower for two hours ( and smashed two bananas) and loved the water on my back. Sitting on the ball and bouncing away under the water was my JAM! To spice things up and keep things moving along (or I hoped would) I laboured on the birth mat, bean bag, used the TENS machine I had hired and the Gas and Air to good effect. Throughout labouring, my Calmbirth breathing that had been a big part of my later pregnancy daily routine was EVERYTHING. I didn’t see it as a coping mechanism in the end and more of a necessity in getting the job (having a baby!) done!
Being reassessed that afternoon, I was 4cm, Bub was still direct OP and his head had started to swell (this is called caput). He was super happy in there, going off his heart rate, so we moved across to the Birth Suite and I got an epidural (I was 6cm by this point) and planned to have a caesarean in the coming hours.
I surprisingly wasn’t disappointed by this plan. I thought I would’ve been, but I wasn’t. When you’re in the moment, labouring away, you realise that birth doesn’t discriminate, you can only control so much, and you really just need to go with the flow.
The epidural was a God send for me. It allowed me to relax, take a second and relax my body for a bit. It also was perfectly timed for Married at First Sight (see top right pic – shameful, I know…to my defence, Raoul loved it more than I did).
The birth suite was having one of those mental nights when all babies decide to kick a stink and all want out, so our caesarean kept getting bumped for Bubs’ that warranted a faster exit.
I was reassessed maybe an hour before we went for the caesar and was 6-7cm, he was still around the wrong way and the plan for the caesar was still in place.
THURSDAY FEBRUARY 22, 2018
Midnight came around and it was our turn – Raoul got into his scrubs (the most animated I’d seen him in a few hours, I think he was fantasising Greys Anatomy style) and we were off.
My epidural was topped up in the anaesthetic bay before entering theatres and then we moved in, and I was transferred (I remember feeling it was more a ‘heave’ ‘ho’ type situation) to the operating table. I remember wanting Raoul and being nervous. Nervous excited, but nervous.
The clip that had been attached to our baby’s head (called a fetal scalp electrode – helps to monitor the baby’s heart rate accurately when they’re on the inside) was being removed by the registrar that was to perform my caesar.
She was quiet and then said, “do you want the good news or the bad news?”
I said bad news. She responded “the bad news is that we’ve just topped up your epidural, the good news is that you’re 9cm and your baby is lower and in an OA position” (this is a perfect pozzy!). I was then asked “what do you want to do? You’re prepped for a caesar, so you can still have the caesarean now if you want it….or….if you want to try for a vaginal birth I will support you in that decision…it’s up to you. I can’t guarantee that you won’t be back here in a few hours, but if you want to give it a go, I’ll support that”. – What a legend Doctor right there, yeah? Looking back I’m still so amazed and grateful that I had a Registrar on that night that was so woman-centred (it would’ve been 1000 times easier for her to have just done the caesar, I would’ve never been the wiser). I’m forever grateful to her.
I was swirling. I remember just wanting Raoul to make the decision for me. I wanted the caesarean because I was over it and wanted to meet our baby, and had mentally seen the finish line, but I also wanted the natural birth…for the recovery, for the babies of the future etc.
Raoul came into the room, beaming like a cheshire cat in his scrub hat, and I broke the latest news. He smiled and said, “the ideal was for a natural birth, let’s give it a go- I’ll support you if you want to go for it”. He made it sound simple, and easy to process, and he was right, we did want it. So we gave it a go.
I waited 50 mins on the table in theatres for the epidural block to come down to a safe level to leave theatres, to then spend 1.5hours in recovery being monitored further.
By 3am we were being wheeled back to Birth Suite and I started to vomit – fully dilated!
They gave me an hour for passive descent (meaning just keep doing what you’re doing, no directed pushing etc., and let baby’s head come down low enough that I then had the urge to push).
My epidural had in the meantime stopped working. Now from a midwife’s perspective, this is perfect timing to regain sensation so you can feel where to channel your energy when pushing and being able to listen to your body. I didn’t feel this way at all!!! I was furious!!! I felt I had been able to handle the ‘pain’ throughout the day well, working my way up with pain relief options. To go from 0-100000 on the pain scale didn’t seem fair and it was a real mind-fuck for me.
The anaesthetist came back but no luck. So with the epidural in situ, I was standing next to the bed and pushing upright – it definitely wasn’t working!
This is going to sounds horrif as a midwife, but I just wanted to get Bub low enough for the vacuum birth. I was beyond exhausted and ready to meet him. My midwife in the following days said I did exactly that, that I got him low enough and then demanded a vacuum (what a nightmare I would’ve been to look after!)
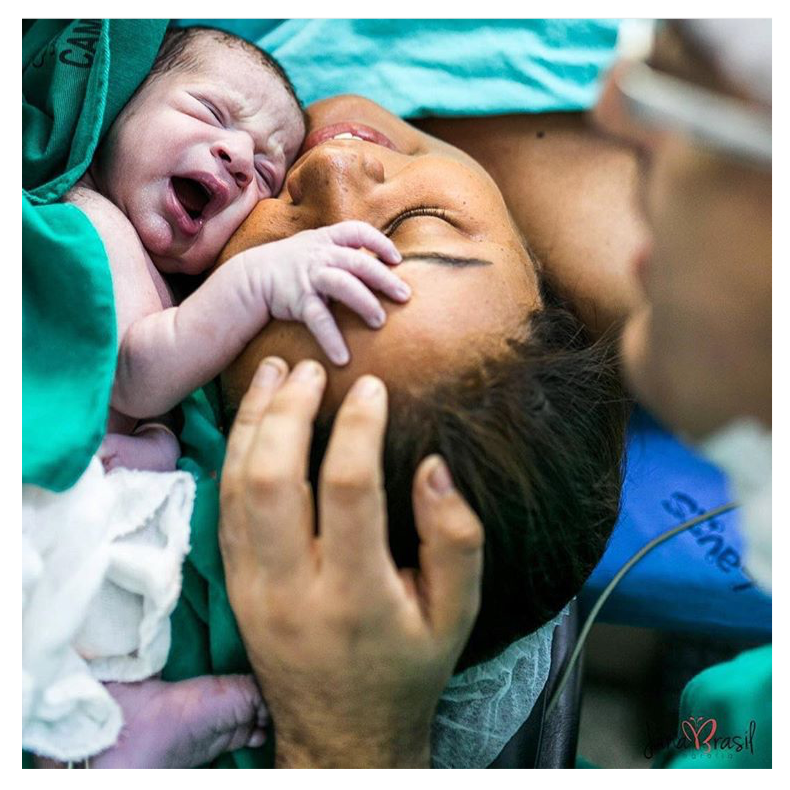
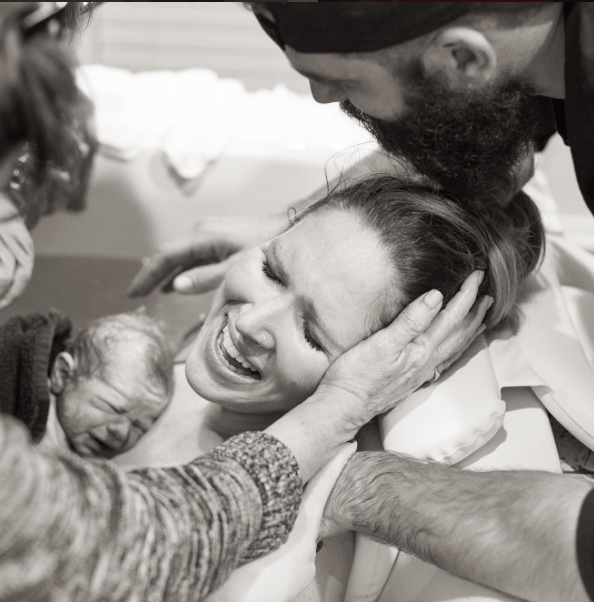
I did end up having a vacuum, and little Syd born at 5:16am. I’d cooked up quite the temperature at 38.6, and Syd was 38.8 so he went straight off to the nursery after a very quick little snuggle.
A few hours later, after a shower, I met him again, and he had a feed.

We left hospital 2 days later.

It was an eventful few days but looking back I feel so incredibly lucky to have had the information, the preparation and the support to head into the unknown that is birth.
We all just want the best outcome possible at the end of the day.
My ideals changed so quickly in the moment – and I was okay with that. However I stand by my original ethos that the best birth plan is no birth plan at all and rather an informed pregnancy to make the best decisions you can in the moment. In the end, that’s what we did, and whether I’d had the caesar or not, I was happy that I had given it my all, and that’s all you really can do at the end of the day.
To that doctor – I have met woman-centred medical staff over the years, but never have I felt I’ve seen one so in the woman’s corner. Thankyou. You literally have changed my birth journey moving forward.
Raoul was also a champ – he gave a cracker massage, never wavered in support and knew exactly what to say at the right time. A+ !





















 Evidence-based info for parents-to-be.
Follow us @winniewagtail
Evidence-based info for parents-to-be.
Follow us @winniewagtail


















